Blincyto® (blinatumomab) is a monoclonal antibody indicated as a treatment for relapsed or refractory B-cell precursor acute lymphoblastic leukaemia (ALL) in adults and children.
The drug was originally developed by US-based biotechnology company Micromet in association with MedImmune, a wholly owned subsidiary of AstraZeneca. After Micromet was acquired by Amgen in January 2012, Amgen assumed production of the drug.
Blinatumomab was granted orphan drug designation in February 2006 by the US Food and Drug Administration (FDA) for some types of indolent B cell lymphoma, acute lymphoblastic leukaemia and chronic lymphocytic leukaemia.
The European Medicines Agency (EMA) granted orphan drug designation to blinatumomab for the treatment of chronic lymphocytic leukaemia and mantle cell lymphoma. In July 2009, the EMA also granted orphan drug designation to blinatumomab for the treatment of ALL.
The drug received accelerated approval from the FDA in March 2018 and full marketing authorisation from the European Commission in June 2018.
In July 2017, the FDA initially granted full approval to the drug to treat patients with Philadelphia chromosome (Ph) negative and positive relapsed or refractory positive B-cell precursor ALL.
Potential of blinatumomab to treat lymphoma
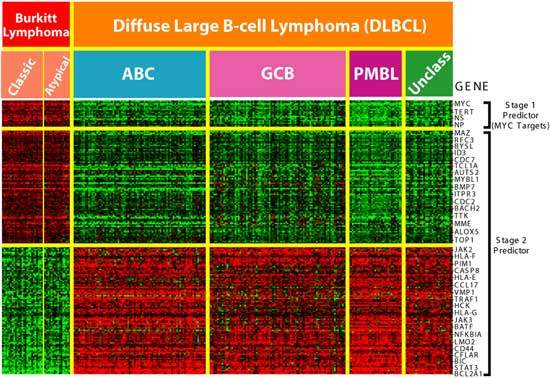
Lymphoma is a form of blood cancer that arises in the lymphatic system. In lymphoma, lymphocytes start reproducing in an abnormal manner, pile up and gather in some parts of the lymphatic system such as the lymph nodes. The affected lymphocytes lose their infection-fighting capabilities, making them vulnerable to infection.
Although the exact causes of lymphoma are still unknown, several factors have been linked to an increased risk of developing lymphoma. These factors include age, infection with human immunodeficiency virus (HIV), medical conditions weakening the immune system, exposure to toxic chemicals, and genetics. It is unclear, however, as to what role these factors play in the development of lymphoma.
According to the National Cancer Institute, around 5,960 people in the US will be diagnosed with ALL in 2018. Of these, around 1,470 will die from the disease.
Blincyto mechanism of action
Blincyto is a monoclonal antibody (a type of protein) that contains four immunoglobulin variable domains arranged into a single polypeptide chain.
Two of the variable domains build the binding site for CD19, a cell surface antigen found on many B cells and B tumour cells. The other two variable domains build the binding site for the CD3 complex on T cells.
The CD3 complex is responsible for activating the T cells. Micromet used its Bispecific T Cell Engager (BiTE) technology to create Blincyto by fermentation with eukaryotic cells.
Blincyto works by targeting CD19 on B cells and using T cells to eliminate the cancer cells. The drug is available for injection as 35mcg of lyophilised powder in a single-dose vial for reconstitution.
Clinical trials on Blincyto
The FDA’s previous approval was based on a single-arm clinical trial, which studied Blincyto’s efficacy in 86 patients with Philadelphia chromosome-positive ALL based on the achievement of an undetectable minimal residual disease (MRD) method. This method could detect at least one cancer cell in 10,000 cells in the bone marrow after treatment with one cycle of Blincyto.
A total of 70 patients achieved undetectable MRD and almost 50% of patients remained alive and in remission for up to 22.3 months. Haematological relapse-free survival was also evaluated during the study.
The most common side effects reported in patients during the clinical trial include infections, fever, headache, infusion-related reactions, neutropenia, anaemia, low levels of platelets, neutropaenia and fever.
Blincyto’s safety profile in 405 adult patients with Ph-negative relapsed or refractory B-cell precursor ALL was studied in TOWER, a Phase III randomised, open-label, active-controlled clinical study.
The drug showed significant improvement in median overall survival (OS) compared to standard-of-care chemotherapy during the study. The median OS of patients receiving Blincyto was 7.7 months, compared with only four months for those on chemotherapy.